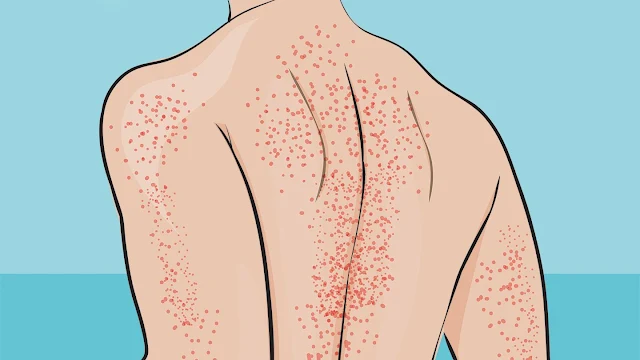
INTRODUCTION: Thrombocytopenia which is a condition of low platelet count, is the most common cause of abnormal bleeding.
PATHOPHYSIOLOGY: Thrombocytopenia can result from decreased production of platelets within the bone marrow or from increased destruction or consumption of platelets.
CAUSES: Causes include failure of production as a result of hematologic malignancies, myelodysplastic syndromes, metastatic involvement of bone marrow from solid tumors, certain anemias, toxins, medications, infections, alcohol, and chemotherapy; increased destruction as a result of idiopathic thrombocytopenia purpura, lupus erythematosus, malignant lymphoma, chronic lymphocytic leukemia, medications, infections, and sequestration; and increased utilization, such as results from disseminated intravascular coagulopathy (DIC).
CLINICAL MANIFESTATIONS: With platelet count below 50,000/mm3 : bleeding and petechiae. With platelet count below 20,000/mm3 : petechiae, along with nasal and gingival bleeding, excessive menstrual bleeding, and excessive bleeding after surgery or dental extractions. With platelet count below 5,000/mm3: spontaneous, potentially fatal central nervous system hemorrhage or gastrointestinal hemorrhage.
ASSESSMENT AND DIAGNOSTIC FINDINGS: Bone marrow aspiration and biopsy, if platelet deficiency is secondary to decreased production. Increased megakaryocytes (the cells from which platelets originate) and normal or even increased platelet production in bone marrow, when platelet destruction is the cause.
MEDICAL MANAGEMENT: The management of secondary thrombocytopenia is usually treatment of the underlying disease. Platelet transfusions are used to raise platelet count and stop bleeding or prevent spontaneous hemorrhage if platelet production is impaired; if excessive platelet destruction is the cause, the patient is treated as indicated for idiopathic thrombocytopenia purpura.
For some patients a splenectomy can be therapeutic, although it may not be an option for other patients for example, patients in whom the enlarged spleen is due to portal hypertension related to cirrhosis.
RELATED;