INTRODUCTION:
For an infectious disease to perpetuate there has to be a
reservoir of microorganism from where the causative agent should be
transmitted to a susceptible host either directly or through the
agency of a vehicle or a vector.SOURCE
AND RESERVOIR: The source of infection is the person, animal,
object or substance from which an infectious agent passes or
disseminates to the host whereas a reservoir is defined as any
person, animal, arthropod, plant, soil or substance (or combination
of these) in which an infectious agent lives and multiplies. These
can be of three types: 1) Humans 2) Animals 3) Non-living
substances. Humans For infectious diseases of human beings, man is
the most important reservoir. He may be a case
or a carrier.
HUMAN
CASE: A case may be having a clinical disease or subclinical
infection which remains unmanifested or abortive. In latter, the
disease agent may multiply in the host but does not manifest itself
by signs and symptoms.
HUMAN
CARRIERS: Some microorganisms do not get completely eliminated
from the host after natural cycle of disease or after treatment. Such
persons become carriers of the agents. A
carrier therefore
is defined as an infected person or animal that harbours a specific
infectious agent in the absence of overt clinical signs and serves as
a potential source of infection for others.
Though
carriers are less infectious than cases, they carry greater
epidemiological importance because of the prolonged duration for
which they can silently excrete organisms. The carriers can be: 1)
incubatory 2) convalescent or 3)
healthy. Depending upon the duration of excretion of
microorganisms they can be designated as: 1) temporary (acute) or
2) chronic
carriers.
The
incubatory and convalescent carriers are usually temporary whereas
chronic carriers are otherwise healthy individuals. Chronic carrier
state occurs in various diseases notably typhoid fever and hepatitis
B. Hepatitis B
ANIMALS:
Animals and birds can also pass on microorganisms to man. These
may also manifest as case or exist as carriers. The diseases which
are naturally transmissible between man and animals are called as
zoonoses. These diseases are
of great importance in countries where a close contact between man
and animals is inevitable such as occurs in rural areas of India and
Sub-Saharan Africa. Some of the important zoonotic infections are
rabies; plague, brucellosis, leptospirosis, hydatidosis. Brucellosis
NON-LIVING
SUBSTANCES: Soil and inanimate objects can also occur as
reservoir of some microorganisms such as causative agents of
infectious tetanus, anthrax, hookworm disease and mycetoma.
MODES
OF TRANSMISSION: The microorganisms can be transmitted to human
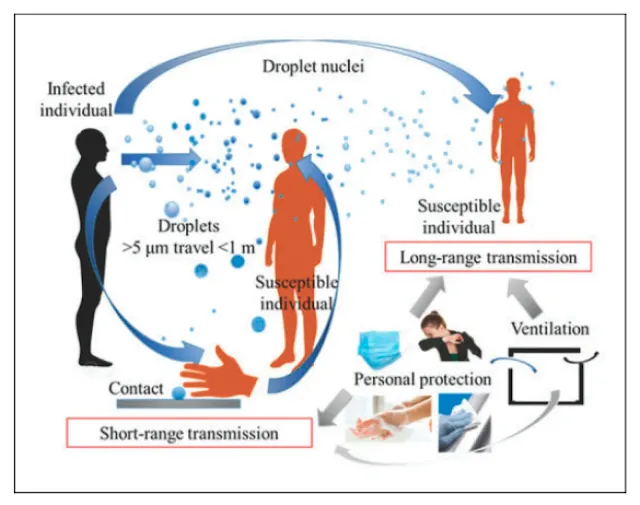
beings directly or indirectly. Direct transmission occurs through: 1)
Contact with man, animal or inanimate objects. 2) Droplet
infection 3) Breach of skin or mucous membrane 4) Transplacental
and congenital.
The
indirect transmission is possible by any of the
following mechanisms; 1) Vehicles (water, food etc.). 2) Vectors
(mechanical or biological). 3) Air (droplet or dust). 4) Fomites.
5) Unclean hands and fingers.
MECHANISM
OF INFECTION: To produce infection in man a microbe has to gain
entry into the host. The most frequent portals of entry are the
respiratory tract, the gastrointestinal tract and breaks in the
superficial mucous membranes and skin. From the portal of entry the
parasite may spread directly through the tissues or may proceed via lymphatic
channels to the blood stream, which distributes it widely and permits
it to reach tissues particularly suitable for its multiplication.
Nevertheless, for the perpetuation of a parasitic species a
satisfactory portal of exit of the parasite from the host and an
effective mechanism for transmission to new hosts are also of
paramount importance.
DEVELOPMENT
OF DISEASE: Once the microorganism overcomes the defences of the
host, development of infectious disease follows a sequence of events.
Period
of Incubation: This is the time interval between the actual
infection and the appearance of first clinical feature.
Prodromal
Period: This relatively short period follows incubation period in
some diseases. It is characterised by mild early symptoms such as
general aches and malaise.
Period
of Illness: This is the acute phase of illness characterised by
typical clinical features of the infectious disease.
Period
of Decline: During this period the signs and symptoms subside.
The fever decreases and the feeling of malaise diminishes
Period
of Convalescence: The person regains strength during this period
and body
returns to pre-diseased state.
LOCAL
OR GENERALISED INFECTIONS: An infection may be restricted to the
point of entry (local)
or may spread throughout the body (generalized).
Generalised
Infections: Bacteraemia,
septicaemia and pyaemia are some of the generalised
infections which spread through blood:
Bacteraemia:
Bacteraemia is defined as the circulation of bacteria in the
blood. It may be transient or of
long duration depending
upon the duration for which bacteria are present
in the blood. Transient bacteraemia
is a frequent event which occurs even in healthy individuals
while chewing, brushing of teeth and straining while passing stools.
Bacteraemia of long duration occurs
with pathogenic organisms such as Salmonella typhi and Brucella and is essential
for the initiation of disease process.
Septicaemia:
This is a condition in which bacteria circulate and multiply in
the blood, form toxic products and cause high swinging type of fever.
This can be due to both endotoxin
as well as exotoxin producing organisms.
RELATED;
1.
SEPTIC SHOCK
2.
FEVERS
3.
BACTERIA TOXINS
4.
VIRULENCE OF MICROORGANISMS
5. MEDICAL MICROBIOLOGY
REFERENCES