INTRODUCTION:
Spinal
cord injuries (SCIs) are a major health problem. Most SCIs result
from motor vehicle crashes. Other causes include falls, violence
especially primarily from gunshot wounds, and recreational sporting
activities. Half of the victims are between 16 and 30 years of age;
most are males. Another risk factor is substance abuse (alcohol and
drugs). There is a high frequency of associated injuries and medical
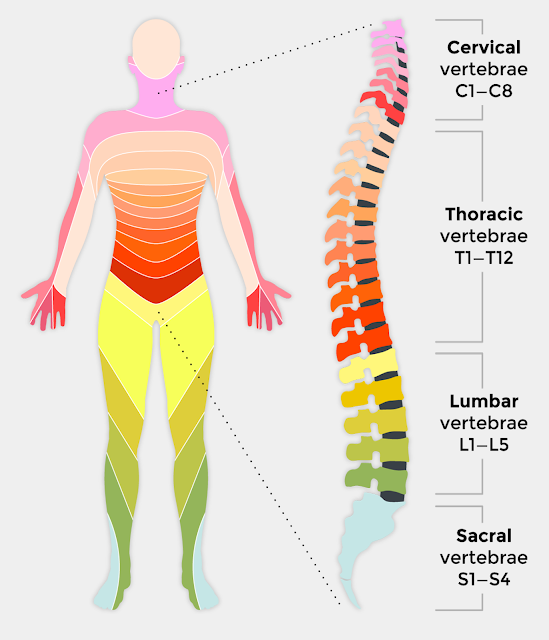
complications. The vertebrae most frequently involved in SCIs are the
fifth, sixth, and seventh cervical vertebrae (C5–C7), the 12th
thoracic vertebra (T12), and the first lumbar vertebra (L1). These
vertebrae are the most susceptible because there is a greater range
of mobility in the vertebral column in these areas. Damage to the
spinal cord ranges from transient concussion (patient recovers
fully), to contusion, laceration, and compression of the cord
substance (either alone or in combination), to complete transection
of the cord (paralysis below the level of injury). Injury can be
categorized as primary (usually permanent) or secondary (nerve fibers
swell and disintegrate as a result of ischemia, hypoxia, edema, and
hemorrhagic lesions). Whereas a primary injury is permanent, a
secondary injury may be reversible if treated within 4 to 6 hours of
the initial injury. The type of injury refers to the extent of injury
to the spinal cord itself. Incomplete spinal cord lesions are
classified according to the area of spinal cord damage: central,
lateral, anterior, or peripheral. A complete SCI can result in
paraplegia (paralysis of the lower body) or tetraplegia (formerly
quadriplegia— paralysis of all four extremities).
CLINICAL
MANIFESTATIONS: The
consequences of SCI depend on the type and level of injury of the
cord.
Neurologic
Level: The
neurologic level refers to the lowest level at which sensory and
motor functions are normal. Signs and symptoms include the following:
Total sensory and motor paralysis below the neurologic level. Loss
of bladder and bowel control (usually with urinary retention and
bladder distention). Loss of sweating and vasomotor tone. Marked
reduction of BP from loss of peripheral vascular resistance. If
conscious, patient reports acute pain in back or neck; patient may
speak of fear that the neck or back is broken.
Respiratory
Problems: Related
to compromised respiratory function; severity depends on level of
injury. Acute respiratory failure is the leading cause of death in
high cervical cord injury.
ASSESSMENT
AND DIAGNOSTIC METHODS: Detailed
neurologic examination, x-ray examinations (lateral cervical spine
x-rays), computed tomography (CT), magnetic resonance imaging (MRI),
and ECG (bradycardia and asystole are common in acute spinal
injuries) are common assessment and diagnostic methods.
COMPLICATIONS:
Spinal
shock, a serious complication of SCI, is a sudden depression of
reflex activity in the spinal cord (areflexia) below the level of
injury. The muscles innervated by the part of the cord segment
situated below the level of the lesion become completely paralyzed
and flaccid, and the reflexes are absent. BP and heart rate fall as
vital organs are affected. Parts of the body below the level of the
cord lesion are paralyzed and without sensation.
EMERGENCY
MANAGEMENT: Immediate
patient management at the accident scene is crucial. Improper
handling can cause further damage and loss of neurologic function.
Consider any victim of a motor vehicle crash, a diving or contact
sports injury, a fall, or any direct trauma to the head and neck as
having an SCI until ruled out. Initial care includes rapid
assessment, immobilization, extrication, stabilization or control of
life-threatening injuries, and transportation to an appropriate
medical facility. Maintain patient in an extended position (not
sitting); no body part should be twisted or turned. The standard of
care is referral to a regional spinal injury center or trauma center
for treatment in first 24 hours.
MEDICAL
MANAGEMENT: Acute
Phase Goals of management are to prevent further SCI and to observe
for symptoms of progressive neurologic deficits. The patient is
resuscitated as necessary, and oxygenation and cardiovascular
stability are maintained. High-dose corticosteroids
(methylprednisolone) may be administered to counteract spinal cord
edema. Oxygen is administered to maintain a high arterial PaO2.
Extreme care is taken to avoid flexing or extending the neck if
endotracheal intubation is necessary. Diaphragm pacing (electrical
stimulation of the phrenic nerve) may be considered for patients with
high cervical spine injuries. SCI requires immobilization, reduction
of dislocations, and stabilization of the vertebral column. The
cervical fracture is reduced and the cervical spine aligned with a
form of skeletal traction (using skeletal tongs or calipers or the
halo-vest technique). Weights are hung freely so as not to interfere
with the traction. Early surgery reduces the need for traction. The
goals of surgical treatment are to preserve neurologic function by
removing pressure from the spinal cord and to provide stability.
MANAGEMENT
OF COMPLICATIONS:
Spinal
and Neurogenic Shock: Intestinal
decompression is used to treat bowel distention and paralytic ileus
caused by depression of reflexes. This loss of sympathetic
innervation causes a variety of other clinical manifestations,
including neurogenic shock signaled by decreased cardiac output,
venous pooling in the extremities, and peripheral vasodilation.
Patient who does not perspire on paralyzed portion of body requires
close observation for early detection of an abrupt onset of fever.
Body defenses are maintained and supported until the spinal shock
abates and the system has recovered from the traumatic insult (up to
4 months).
RELATED;
1. THE CENTRAL NERVOUS SYSTEM
2. THE ENTERIC NERVOUS SYSTEM
3. ACTIVATION OF A NERVE IMPULSE
4. BACK PAIN
REFERENCES










.png)